Study of graft arteries – Background
Coronary artery bypass surgery
Normal heart function depends on adequate blood supply to the heart. The coronary arteries supply the heart with blood. Over time, these vessels can become narrowed and this may eventually lead to an inadequate blood supply to meet the heart’s demands. If the problem cannot be managed successfully with medical therapy, the standard treatment is coronary artery bypass graft (CABG) surgery. This is a surgical procedure in which a vein or artery is used to bypass a blockage in the coronary arteries. Initially only leg veins were used as bypass vessels or grafts. Currently the artery from behind the breastbone (internal thoracic artery) and the forearm artery (radial artery) are often used as bypass vessels.
The internal thoracic artery (ITA) is usually used because it is unlikely to be blocked, that is, it has good patency. Some early trials suggested that the radial artery (RA) might be suitable for CABGs as its patency is as good as, or better than, the ITA. However, good patency is only one aspect of the suitability of an artery for CABG. The potential for pathological changes, such as developing atherosclerosis, is also important. Atherosclerosis is the degeneration of artery walls. There is little information about the incidence of atherosclerosis in the RA.
Objective
To compare the incidence of disease in the ITA and RA of patients undergoing CABG surgery.
Data collection methods
One hundred and fifty patients, 132 men and 18 women, participated. A segment of the ITA and a segment of the RA was collected from each patient during CABG surgery.
Data were obtained by three methods:
- Information about potential risk factors for atherosclerosis was obtained by interviewing patients.
- Histopathology of ITA and RA segments provided information about the presence of abnormalities in the artery.
- Morphometric analysis of ITA and RA segments provided measurements related to the severity of disease in the artery. Note that morphometric analysis was carried out on 110 pairs of arteries; 40 pairs were excluded because risk factor details were incomplete for those patients or because the arteries were distorted during surgery or in preparation for morphometric analysis.
Some lifestyle and genetic characteristics increase the likelihood of developing atherosclerosis. For example, the risk of developing atherosclerosis increases with age, and is higher for men than for women. Other risk factors include being a diabetic, smoking cigarettes, having high blood pressure (hypertension) or high blood cholesterol (hypercholesterolemia), or having other kinds of vascular diseases (peripheral vascular disease or cerebrovascular disease).
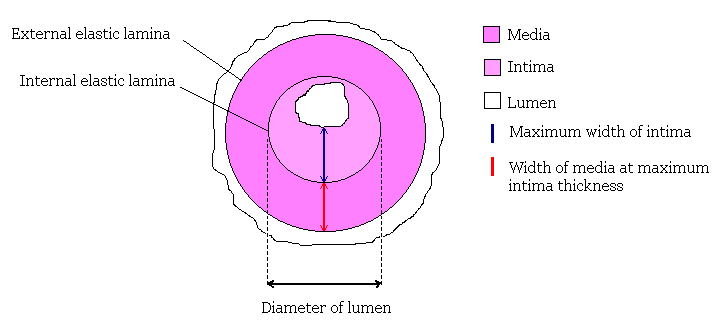
A pathologist can identify various arterial abnormalities by examining cross-sections of the artery under magnification. Below is a figure showing a cross-section of an artery. Normally, the intima rests on the internal elastic lamina; intimal thickening is identified if extra tissue or cells are observed between the intima and the internal elastic lamina. Calcification or hardening of the media can also be noted. Atherosclerosis is indicated by the presence of cholesterol or foamy white blood corpuscles.
The three arterial abnormalities, intimal thickening, medial calcification and atherosclerosis can lead to impaired blood flow through the artery.
Morphometric analysis provides a way of quantifying the degree of intimal thickening and atherosclerosis. The analysis in this study was based on the most severely diseased part of an artery. Morphometric analysis provides a measures of various characteristics of an artery which are combined to provide indices of disease severity.
The 3 main indices used were:
- Percentage of luminal narrowing;
- Intimal thickness index, and;
- Intima-to-media ratio.
Higher values of each of these indices indicate more severe disease. Luminal narrowing, intimal thickening and a high intima-to-media ratio mean that blood flow will be impaired.
|
|
|
|
|
Article
Ruengsakulrach, P., Sinclair, R., Komeda, M., Raman, J., Gordon, I., & Buxton, B. (1999) Comparative histopathology of radial artery versus internal thoracic artery and risk factors for development of intimal hyperplasia and atherosclerosis. Circulation, 100(19), II-139 – II-144.



